Capnography tips
Tips on using capnography- Abnormal values and shapes
The following guidelines can be used to assess abnormal capnograms. However, a thorough understanding of underlying principles of capnography will to help you to maximize the benefit of capnography in rectifying a clinical abnormality during anesthesia.
1. Rule out technical causes of abnormal capnograms. The guidelines listed in the previous two pages should help in minimizing abnormal waveforms as a result of technical errors. The author is privileged to have been called when abnormal capnograms were observed in the operating rooms. The most frequent abnormal capnograms which were as a result of technical problems included a loose connection between the sampling tube and the monitor, cracked connection at the monitor end of sampling tube, and sticking unidirectional valves of the closed circuit. The abnormal capnograms observed are as follows.
| Sticking Inspiratory unidirectional valve | Loose connection between the sampling tube and the monitor |
 |
 |
| Details | Details |
5. Baseline elevation in increased, normal, or low PETCO2 presence suggests rebreathing. A rebreathing can be normal in rebreathing circuits, but definitely abnormal in a closed circuit anesthesia and suggests exhaustion of soda lime or defective unidirectional inspiratory or expiratory valves.
6. A sudden elevation of baseline and PETCO2 usually suggests contaminated monitors.
7. If capnogram is abnormal in shape, proceed to analyze starting from baseline (phase I), upstroke (phase II), alveolar plateau (phase III), and descending limb (phase 0). Commonly seen abnormal capnograms
Phase I: Elevation: Rebreathing
Phase II: Prolongation: Airway obstruction
Phase III: Increased slope: Airway obstruction; Cleft in phase III: Spontaneous effort during controlled ventilation
Phase 0: Descending limb usually makes a nearly 90 angle with an alveolar plateau. An increase in this angle (a sloping descending limb) usually suggests rebreathing.For an atlas of abnormal capnogram details: see Capno-encyclopedia.A sample list of abnormal capnograms is as follows:
| Bronchospasm |
Curare cleft |
 |
 |
| Ripple effect | Contamination |
 |
 |
| Sampling tube leak | Hypoventilation |
 |
 |
| Bain circuit | Apnea |
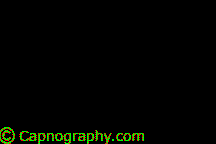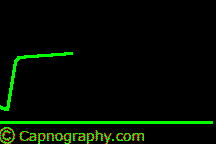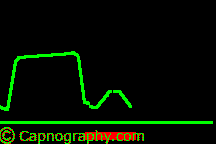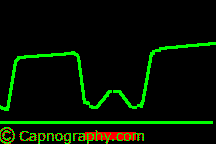 |
 |
| Inspiratory unidirectional valve defect | Spontaneously breathing capnograms in children |
 |
 |

 Twitter
Twitter Youtube
Youtube









