Physiology of capnography
Basic Physiology
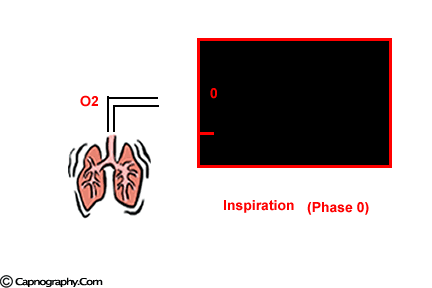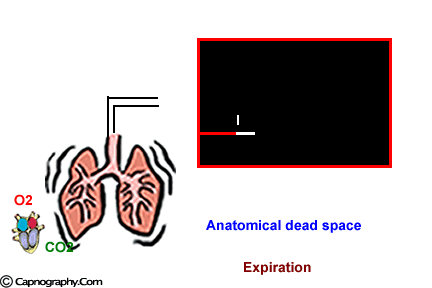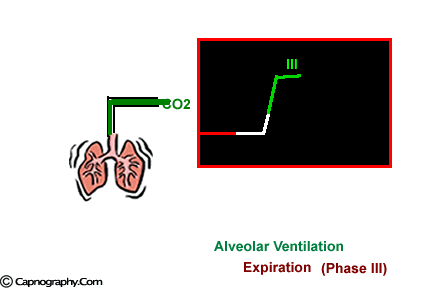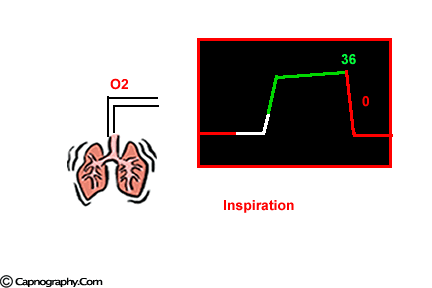
At the end of inspiration, assuming that there is no rebreathing, the airway and the lungs are filled with CO2-free gases. Carbon dioxide diffuses into the alveoli and equilibrates with the end-alveolar capillary blood (PACO2 = PcCO2 = 40 mm Hg). The actual concentration of CO2 in the alveoli is determined by the extent of ventilation and perfusion into the alveoli (V/Q ratio). The alveoli with higher ventilation in relation to perfusion (high V/Q alveoli) have lower CO2 compared to alveoli with low V/Q ratio that would have higher CO2. As one moves proximally in the respiratory tract, the concentration of CO2 decreases gradually to zero at some point. The volume of CO2-free gas is termed respiratory dead space and here there is no exchange of oxygen (O2) and CO2 between the inspired gases and the blood. As the patient exhales, a CO2 sensor at the mouth will detect no CO2 as the initial gas sampled will be the CO2-free gas from the dead space. As exhalation continues, CO2 concentration rises gradually and reaches a peak as the CO2 rich gases from the alveoli make their way to the CO2 sensing point at the mouth. At the end of exhalation, the CO2concentration decreases to zero (base line) as the patient commences inhalation of CO2 free gases. The evolution of CO2 from the alveoli to the mouth during exhalation, and inhalation of CO2 free gases during inspiration gives the characteristic shape to the CO2 curve which is identical in all humans with healthy lungs.1 Any deviation from this identical shape should be investigated to determine a physiological or a pathological cause producing the abnormality.

 Twitter
Twitter Youtube
Youtube









