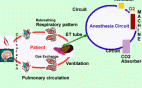
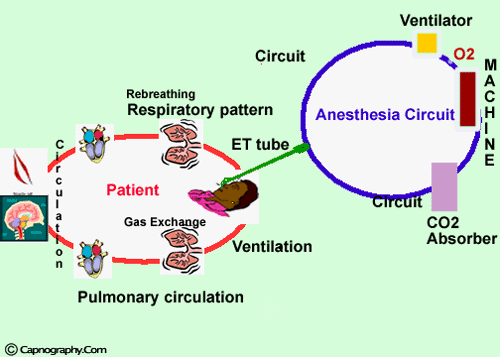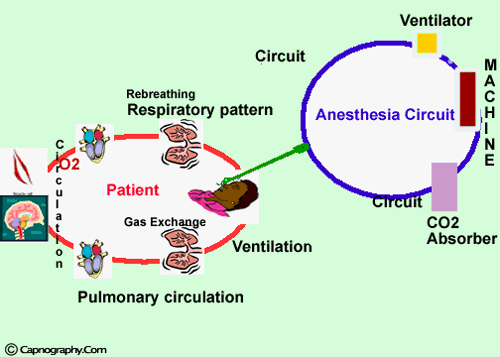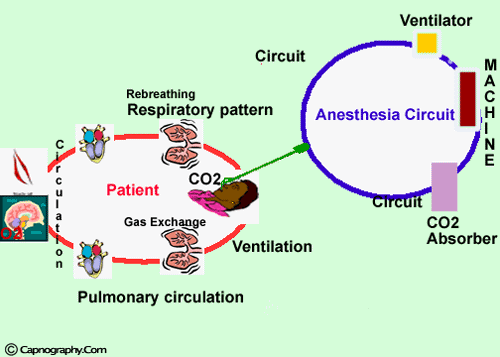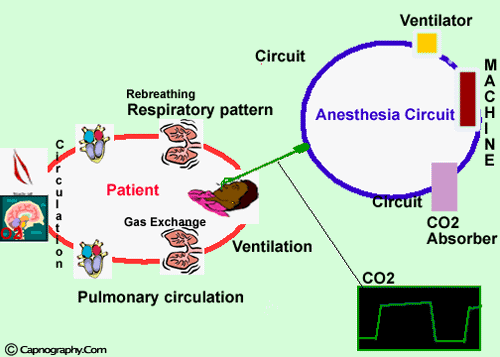
Oxygen and carbon dioxide pathway during anesthesia
Bhavani Shankar Kodali MD
Why Capnography?
Pulse oximeter is a direct monitor to reflect the status of oxygenation of the patient.
- Capnography, on the other hand, is a indirect monitor and helps in the differential diagnosis of hypoxia to enable remedial measures to be taken expeditiously before hypoxia results in an irreversible brain damage.
- Capnography provides information about CO2 production, pulmonary perfusion, alveolar ventilation, respiratory patterns, and elimination of CO2 from the anesthesia circuit and ventilator.
- Capnography has been shown to be effective in the early detection of adverse respiratory events.
- Capnography and pulse oximetry together could have helped in the prevention of 93% of avoidable anesthesia mishaps according to ASA closed claim study.
- Capnography has also been shown to facilitates better detection of potentially life-threatening problems than clinical judgment alone (Cote et al).
In 1978, Holland was the first country to adopt capnography as a standard of monitoring during anesthesia. This is probably due to the relentless work of Kalenda and his colleagues. The American Society of Anesthesiologists, as well several other societies ensuring quality of anesthesia care in their respective countries, have also adopted capnography as an integral part of anesthesia monitoring armamentari
The reasons are as follows:
During anesthesia, there is an interplay between two components; the patient and the anesthesia administration device which is usually a circuit and a ventilator. The critical connection between the two components is either an endotracheal tube, LMA or a mask and the CO2 is typically monitored at this junction. In expired respiratory gases, capnography directly reflects the elimination of CO2 by the lungs to the anesthesia device. Indirectly, it reflects the production of CO2 by tissues and the circulatory transport of CO2 to the lungs. Thus capnography is an important non-invasive technique that provides information about CO2 production, pulmonary perfusion and alveolar ventilation, respiratory patterns as well as elimination of CO2 from the anesthesia circuit and ventilator. Capnography provides a rapid and reliable method to detect life-threatening conditions (malposition of tracheal tubes, unsuspected ventilatory failure, circulatory failure and defective breathing circuits) and to circumvent potentially irreversible patient injury. Studies on the evaluation of anesthesia accidents and related injuries have demonstrated that adverse respiratory events such as hypoventilation, esophageal intubation and circuit disconnection represent a major source of patient injury and financial liability in anesthetic practice. Capnography has been shown to be effective in early detection of these adverse events.

Further reading:
* Cote CJ et al Anesthesiology 1991;74:980-7.
* Kalenda Z. Mastering infrared capnography. The Netherlands:Kerckebosch-Zeist, 1989.
* Caplan RA et al 1990;72:828-33 Cooper JB et al 1984;60:34-42.
Eichhorn JH. Anesthesiology 1989;70:572-7.
* Tinker JH et al. Anesthesiology 1989;71:541-6.
* Birmingham PK et al. Anesth Analg 1986;65:886-9
* Linko K et al. Acta Anesthesiol Scand 1983;27:199-202.

 Twitter
Twitter Youtube
Youtube