Physiology of capnography
| Volume Capnogram / Expirogram/ SBTCO2CO2 Curve | Time Capnogram |
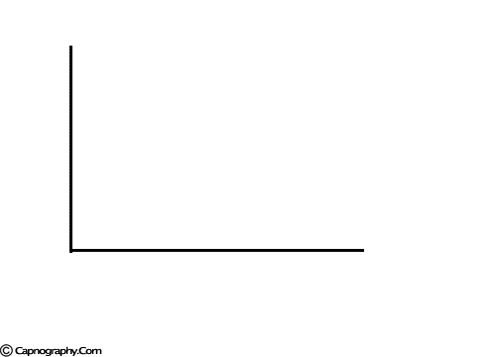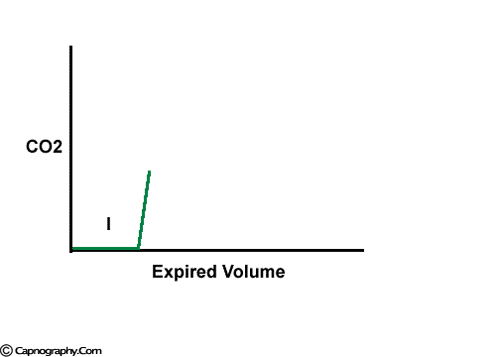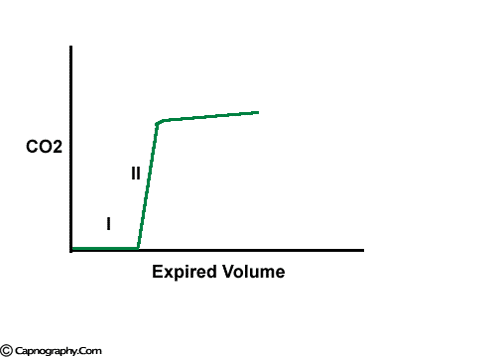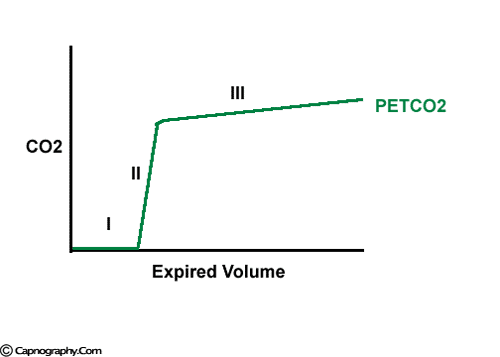 |
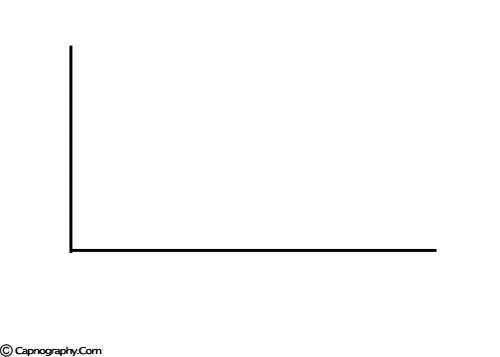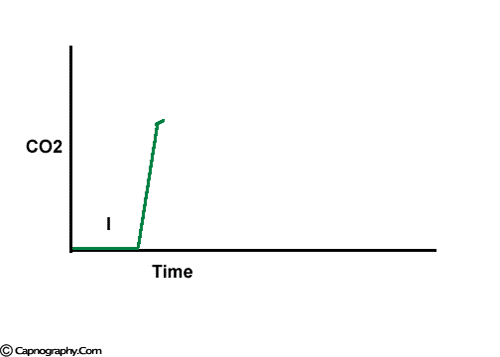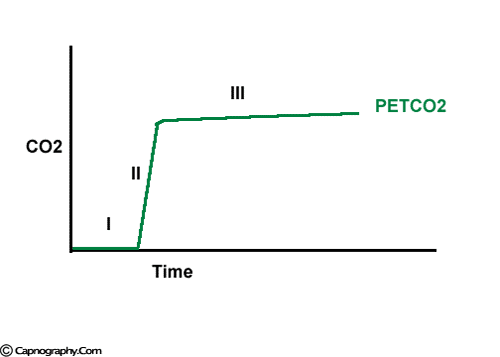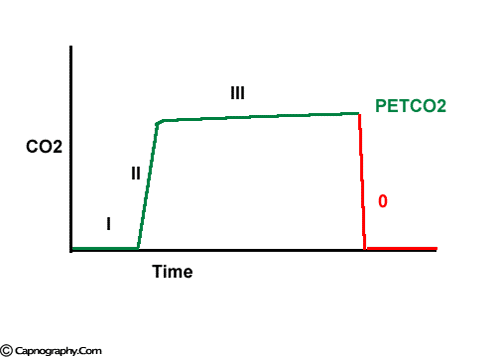 |
Time capnography is simple, popular and adequate for clinical use
h6: There is no inspiratory segment in a volume capnogram
The expiratory segment is divided into three phases
Phase III of a volume capnogram is a better representation of V/Q status of lung than the phase III of time capnogram
Carbon dioxide concentration can be plotted against time (time capnogram) or expired volume (SBT-CO2 curve / Volume capnogram / CO2 expirogram / CO2 spirogram) during a respiratory cycle.1-5 A volume capnogram has only an expiratory segment. There is no inspiratory segment in a volume capnogram. Whereas, a time capnogram has both inspiratory (0) as well as expiratory segment. The expiratory segment of a volume capnogram is divided into three phases, phase I, II, and III.3,4
Advantages of time capnography:
1. Simple and convenient:
2. Monitor non-intubated patients
3. Monitors dynamics of inspiration as well as expiration:
1. Simple and convenient:
The time capnogram is convenient and adequate for clinical use; it is the method most commonly used by capnographs. More elaborate equipment is necessary for plotting SBT-CO2 trace. The CO2 analyzer should be designed to operate with the ventilator, which provides a flow signal and a timing pulse. A computer relates the the instantaneous CO2 signals to expired volume and an SBT-CO2 curve is plotted.3
2. Monitor non-intubated patients:
The CO2 analyzer used in SBT-CO2 tracings are mainstream capnometers, where the cuvette containing the CO2 sensor is inserted between the endotracheal tube and breathing circuit. Hence, endotracheal intubation is required for plotting an SBT-CO2 curve, whereas a time capnogram does not require a ventilator and can be used to monitor spontaneous ventilation without breathing through the ventilator. This is because time capnographs make use of main-stream sensors or side stream sensors. Time capnographs with side-stream sensors have the sensor located in the main unit itself; the sample of gas is aspirated from the patient’s airway, via a tiny pump, through a 6-ft capillary tube, into the unit. This enables time capnography to monitor non-intubated patients, as the sampling of respired gases is obtained from the nasal cavity using nasal adapters.
3. Monitors dynamics of inspiration as well as expiration: Time capnography can be used to monitor the dynamics of expiration as wellasinspiration, whereas the SBT-CO2 curve monitors expiration exclusively.
Disadvantages of time capnography:
1. Poor estimation of V/Q status of the lung
2. Can not be used to estimate components of physiological deadspace.
1. Poor estimation of V/Q status of the lung.
The V/Q status of the lung is more accurately reflected in the slope of phase III in an SBT-CO2 trace than in that of a time capnogram, in which the gradient of the phase III slope is usually less obvious (see figure above). This may be because a smaller volume of expired gases (approximately the final 15%) occupies half the time available for expiration, so that a similar change in FCO2 is distributed over a greater length of time in the time capnogram than in the SBT-CO2 trace.3,4
2. Components of physiological deadspace cannot be determined: /h14: Although the time capnogram grossly can be related to a tidal volume and its components, thephysiological deadspace, CO2 output, the components of a tidal volume cannot be determined from a time capnogram as currently recorded, which is further discussed in the following physiology section.
* References
1. Bhavani Shankar K, Moseley H, Kumar AY, Delph Y. Capnometry and anaesthesia. Review articel. Can J Anaesth 1992;39:517-32.
2. Bhavani Shankar K, Kumar AY, Moseley H, Hallsworth RA. Terminology and the current limitations of time capnography. J Clin Monit 1995;11:175:82.
3. Fletcher R. The single breath test for carbon dioxide. Thesis, Lund, 1980.
4. Fletcher R, Jonson B, Cumming G, Brew J. The concept of deadspace with special reference to the single breath test for carbon dioxide. Br J Anaesth 1981;53:77-88.
5. Breen PH, Bradley PJ. Carbon dioxide spirogram (but not capnogram) detects leaking inspiratory valve in a circle circuit. Anesth Analg 1997;85:1372-6.

 Twitter
Twitter Youtube
Youtube









